As the pandemic shrinks fiscal space, will governments prioritize nutrition funding?
[Editor’s Note: This is a follow-up to an earlier post on how the COVID-19 pandemic is affecting overall funding for nutrition, and as a follow-up on domestic financing for nutrition that looked at trends between 2015 and 2016.]
The current COVID-19 pandemic is posing risks to resource mobilization for nutrition, as noted in our previous blog. This includes significant risks to social sector funding as country governments and donors face more constrained budgets while dealing with emergency response efforts at the same time. There is reason to believe that both donor and domestic financing for health will fall — resulting in an urgent need for governments to protect nutrition from potential budget cuts in order to sustain progress toward nutrition goals.
But can we expect nutrition funding to be prioritized in this way?
The latest data does not give cause for optimism. We looked at available data on domestic nutrition spending in the health sector and found that government spending has been very low and flat between 2015–2017, which suggests that nutrition spending was not prioritized during a period of modest-to-good economic growth in most low- and middle-income countries. Given the high risk of nutrition budget reductions as a result of the COVID-19 economic crisis, there is a critical need to redouble advocacy efforts around maintaining, if not increasing, funding for critical nutrition programs.
What the data shows pre-pandemic
While data on domestic spending for nutrition is limited, the System of Health Accounts (SHA) reports government expenditures on nutritional deficiencies within the health sector which offers some critical insights. Our previous blog on this topic looking at 2015 and 2016 data suggested that government spending had not risen to the level that we might have hoped.
In this updated blog post, we use the newly released 2017 expenditures data to update our analysis of domestic spending, looking at 42 countries with at least two data points across the three years from 2015 to 2017. Three key messages emerge:
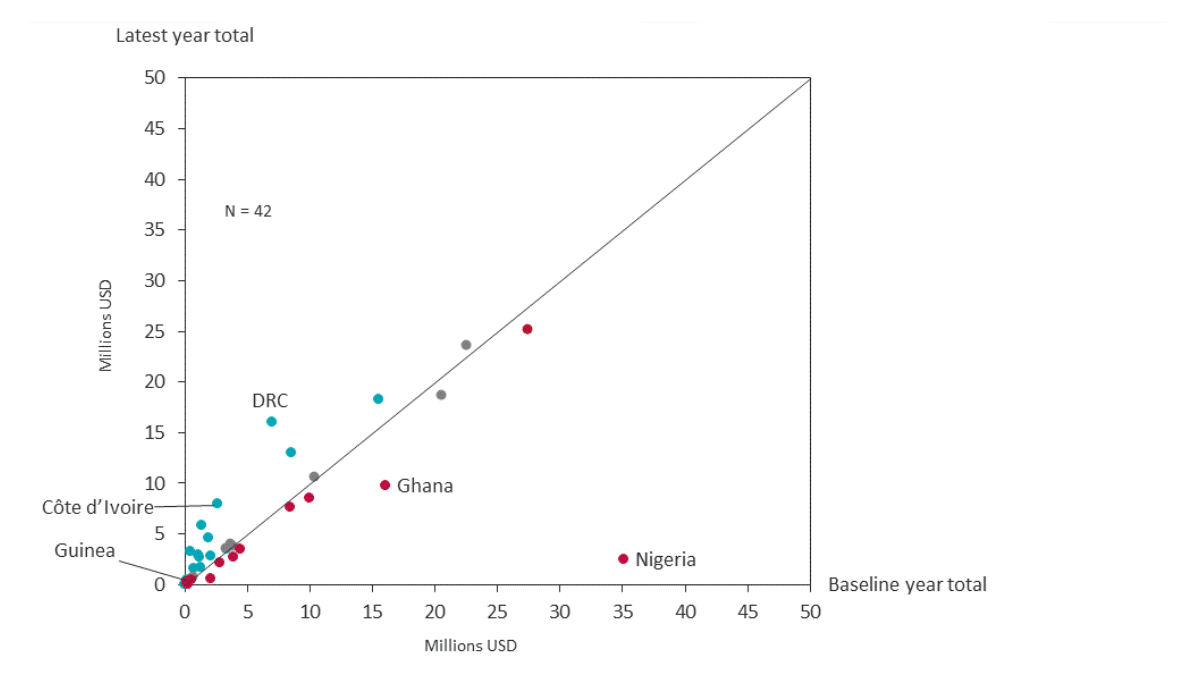
Comparison of 2015-2017 absolute government expenditures on nutritional deficiencies
1. Progress is still flat across countries, with many countries declining spend and just a few countries increasing significantly.
Domestic nutrition spending has not increased at the level needed in the Investment Framework for Nutrition. Out of the 42 countries, 17 countries saw increases in spending since 2015 (>+5% change) while about 16 countries experienced declines (>-5% change) as shown in red in the Figures below. An additional nine countries (shown in grey) remained relatively flat (less than 5% change). Across all countries, the median annual per capita % change was about 1%, which suggests an overall flat rate of change for domestic spending as a whole.
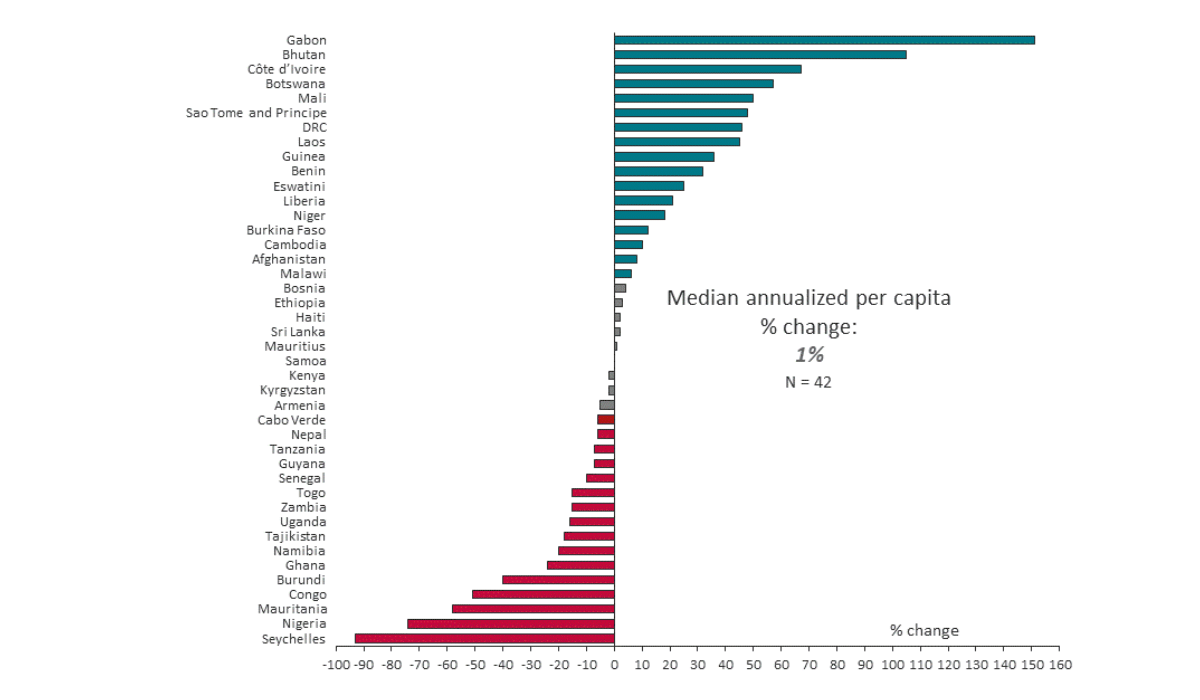
Annualized % change in government expenditures on nutritional deficiencies (per capita) between 2015-2017
2. Some high burden countries have shown positive strides
While trends are flat overall, some high burden countries have increased domestic spending including some who have received little support from donors. For example, Cote d’Ivoire, DRC and Guinea have increased their per capita expenditures each year by 67%, 46%, and 36% respectively (albeit starting from a low base) between 2015 to 2017. In a previous blog on identifying donor orphans — countries that may be receiving less aid than what they should be getting — we saw that these countries, along with other Francophone countries in sub-Saharan Africa, have on average received limited nutrition donor aid relative to their malnutrition burden level and in comparison to other countries in their income group. Such positive stories should be highlighted, and theoretically should catalyze increased donor support if donors are indeed more willing to support countries who have put more “skin in the game” — this narrative is often used to exhort governments to invest in nutrition, but the current circumstances may prove an interesting test to the theory.
3. Some higher income countries are spending less than what might be expected
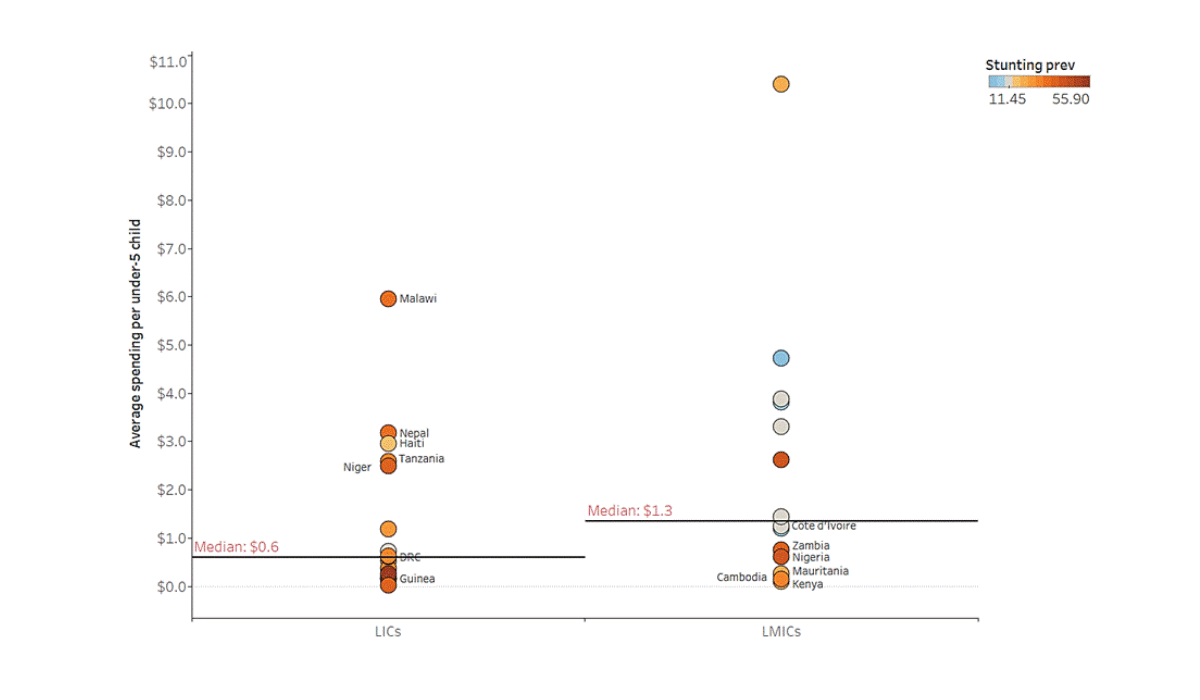
On average across 2015-17, low income countries (LICs) spent about $0.6 per child on nutrition while lower middle-income countries (LMICs) spent about $1.3 per child (nearly double that of LICs). However, as shown above, there is significant variation in nutrition expenditures within income groups. Some LMICs (e.g. Zambia and Nigeria) spend at about the LICs median, while others (e.g. Cambodia, Mauritania, and Kenya) spend even less than the LICs median. While the spend per child from LMICs is typically higher than that of LICs, there are some LMICs that have low levels of spending despite having high burden levels and increased ability to pay for nutrition programming.
Median government expenditure on nutritional deficiencies per under-5 child among LICs and LMICs
What is the pandemic likely to mean for the domestic nutrition financing agenda?
The low and flat levels of domestic funding for nutrition pre-COVID do not bode well for the prioritization of nutrition investments during and in the aftermath of the pandemic because the crisis will result in an even more challenging fiscal environment. A forthcoming study in The Lancet will show that domestic financing for health is likely to fall in times of economic contractions, which can pose significant risks towards nutrition funding. The COVID-19 crisis will significantly increase the number of malnourished people in the world, which makes it imperative to protect nutrition budgets — if not increase them to mitigate the pandemic’s impact on nutrition outcomes.
The Nutrition for Growth (N4G) Summit is the next big opportunity to catalyze renewed government commitments toward nutrition — maintaining current levels of funding and building more nutrition-sensitive systems as part of response and recovery efforts of COVID-19. Though the overall outlook for nutrition financing seems concerning, the pandemic gives us an opportunity to build a post-COVID agenda focused on improving our reach toward more vulnerable, food-insecure populations and mobilizing nutrition-sensitive actions across all sectors (e.g. including nutrition-sensitive components in social protection programs).
Leading up to N4G, we will need to better outline the rationale for why investing in nutrition is more important now than before, and engage countries in making commitments at N4G to ensure that the post-COVID agenda is as nutrition-sensitive as possible.
Photo © USAID